Document Type : Case report
Subjects
Abstract
The coronavirus (COVID-19) pneumonia has been spreading worldwide since February 2019. The most common symptoms are fever, dry cough and fatigue. The virus may affect the lungs, leading to complete opacification and in some cases death. Numerous attempts have been made in early diagnosis through imaging and laboratory tests. Imaging examinations such as conventional x-ray chest radiography and Multi-Detector Computed Tomography (MDCT) are now being used for assessment of the lungs. The authors have presented a case in which signs of COVID-19 were detected in cancer patient undergoing Radiotherapy (RT) using Cone Beam Computed Tomography (CBCT). Cone Beam Computed Tomography is a safe, low dose, three dimensional lung screening evaluation method, in patients suspected for chronic and acute pulmonary diseases and COVID-19.
Keywords: Cone-Beam Computed Tomography, Lung, Radiography, Spiral Cone-Beam Computed Tomography
Introduction
The lungs’ tissue can be affected by several respiratory diseases, including pneumonia and lung cancer. In December 2019, the number of a new type of coronavirus called COVID-19, SARS-CoV-2 (Severe Acute Respiratory Syndrome Coronavirus-2), was extracted from lower respiratory tract from patients presenting with severe pneumonia, fever and fatigue (1). As the number of reported cases of this infection continue to increase, more radiologists may encounter patients with this infection which necessitates a proper imaging modality in order to provide a successful treatment plan. In addition, more diagnostic and treatment facilities are required. Chest x-ray is the most common two-dimensional medical imaging for lung evaluation (2) and in patients confirmed with COVID-19 presence of lung opacities, pleural effusion and pleural calcification can be detected (3); however, the number of lesions of a wide variety of diseases affecting lungs may be missed on a chest radiograph due to the presence of superimpositions and lack of potential for three-dimensional evaluation (4). Multiple studies indicated that chest radiography is less sensitive and less specific than Multidetector Computed Tomography (MDCT) and even if the chest radiograph is normal, MDCT may be necessary in a symptomatic patient (5,6). MDCT plays an increasing role in the diagnosis of chest diseases, especially in patients with unresolving symptoms and can accurately assess the lung parenchyma and chest wall. Qualitative (visual) and quantitative (HU in each region of interest) evaluation of CT axial, coronal and sagittal sections based on underlying increased or decreased pulmonary density, is the main approach for detection and classification of the type of lung abnormalities (7). A number of studies demonstrate the CT appearance of acute severe lower respiratory tract illness in patients positive for COVID-19 which may be bilateral or unilateral and varies and Ground-Glass Opacities (GGOs), air bronchograms, thickening of the adjacent pleura, consolidation, cavitation, discrete nodules, lymphadenopathy, and pleural effusion may be detected (7-9). However, major concerns with MDCT are high patient radiation dose (7 msv) (10), high cost and relative difficulty in access especially during pneumonia pandemics. Although low-dose chest computed tomography (approximately 1.5 msv) is widely used to screen for lung diseases and cancer, as low-level radiation-related carcinogenesis is stochastic in nature, the radiation exposure associated with screening CT has become of concern, despite the utility of CT for lung evaluation (11).
Radiation Therapy (RT) is one of the main treatment options for breast and lung cancers and also lymphomas. Application of image guidance with RT (IGRT techniques) provides online check of the patient anatomy target position and fixes any set-up errors. Nowadays, evaluation of 3-dimensional anatomy of the patient is possible using Cone Beam Computed Tomography (CBCT) imaging in the radiotherapy rooms before each session (12,13). CBCT is a three-dimensional imaging and has considerably lower dose compared to MDCT (14). In addition, CBCT can also be useful for assessment of healthy lungs. Research has shown that although image quality in CBCT is lower than MDCT, retrospective identification of COVID-19 characteristics is feasible. Early diagnosis of COVID-19 is crucial for cancer patients who need radiotherapy since special care should be done for their treatment and prevention of the virus between other patients. Observation of changes related to COVID-19 infection during this process may facilitate earlier testing improving patient management and staff protection (15).
The purpose of this study is to report and describe initially asymptomatic patients in our radiation oncology clinic, who were noted to have imaging changes consistent with SARS-CoV-2 pulmonary changes on CBCT before the onset of symptoms.
Case presentation
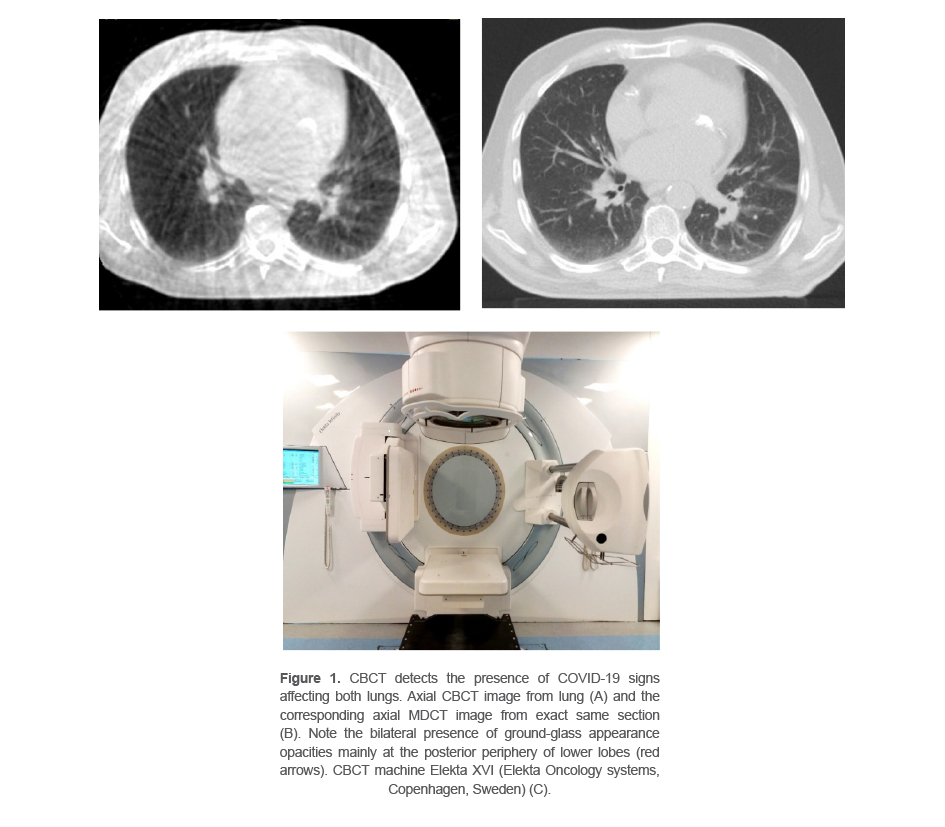
We reported the case of a 30-year-old woman with diagnosed diffused lung B-cell lymphoma cancer referred for adjuvant radiotherapy after chemotherapy to Erfan radiation oncology center, Tehran, Iran. Her non-contrast computed tomography scan for simulation was done after consultation on August 23, 2021. The patient underwent the radiotherapy for 3 weeks using intensity-modulated radiotherapy technique. Treatment was started on August 29. The IGRT protocol used was on-line daily CBCT (CBCT scans were acquired with Elekta XVI (Elekta Oncology systems, Copenhagen, Sweden), version 5.03.). The imaging protocol used for chest CBCT is medium Field of View (FOV) (projected field width and length at isocenter are 27.6727.67 cm2 with 120 kVp). Signs of SARS-CoV-2 findings were observed in her CBCT images on the start of her third week radiotherapy treatment and was referred for consultation and further evaluation. The nasopharyngeal PCR Coronavirus SARS-COV-2 test was positive and her symptoms started in 3 days. The radiotherapy treatment was postponed for 3 weeks and started after her second COVID -19 test became negative. The acquired CBCT is shown in figure 1. Symptoms due to the SARS-CoV-2 were detectable in her images.
Discussion
COVID-19 infection affects patients with underlying diseases to a higher degree, especially patients with cancer. Due to the frequent medical visits of patients with cancer to hospitals and clinics, exposure to COVID-19 poses threat to this vulnerable population (16). In addition, the virus infection may be asymptomatic 80% of the population. However, up to 50% of the infected asymptomatic patients may present radiographic abnormalities in their lung imaging before the onset of symptoms (17). Although MDCT is the main diagnostic tool for diagnosing viral pulmonary infections, in recent years, 3D imaging data from on-treatment CBCT systems has become increasingly available and in patients with thoracic and breast malignancies who are receiving CBCT for setup verification as part of their RT treatment planning, a thorough assessment of lung windows to screen for COVID-19 changes could result in early detection of the infection in asymptomatic patients. Modern radiotherapy linear accelerators (Linacs) are equipped with kilovoltage CBCT imaging systems that produce photon beams of 70 to 150 kVp. The collimators allow for reconstruction of small, medium and large FOV that is wide enough for evaluation of lungs. These images are used for verification of patient setup and omitting the probable geometrical errors before treatment. Given the relatively high proportion of patients with cancer treated in most radiation oncology departments, CBCT imaging presents a unique opportunity for lung evaluation during the COVID-19 pandemic (18) and may facilitate immediate diagnosis of these patients, leading to quarantine and treatment if necessary, with no need for further exposure to the lungs. In addition, there is no need for additional imaging appointments and the concomitant dose is reduced. Recent studies have presented changes associated with COVID-19 disease in these groups of patients peripheral or central GGOs, crazy paving pattern, consolidation, and reverse halo sign with gradual progression in further imaging. Unilateral GGOs are more likely to be seen in asymptomatic patients. CBCT has already been used in interventional medicine and lung biopsies using C-arm CBCT or DynaCT. In the study of Hohenforst-Schmidt et al, DynaCT (CBCT) was utilized as a navigation tool in bronchial biopsy. The results suggested a twofold increase in diagnostic yield of DynaCT guided biopsies in comparison to that of conventional guided biopsies under fluoroscopy, especially in nodules less than 2 cm and significant lower dose to the patient (19). Introducing CBCT units as a low dose, three-dimensional scan in assessing lungs for patients suspected for acute or chronic pulmonary diseases and COVID-19 is practical as chest has high subject contrast (air with -1000 HU adjacent to compact bone with + 3000 HU). The appropriate non-C-arm CBCT machines for chest evaluation needs to provide: 1- supine position with the patient’s body accurately located in the gantry (Figure 2), 2- Large field of view approximately 26 21 mm to best image the anatomy of both lungs in one acquisition, 3- arms should be held up to avoid partial object effect and 4- the diaphragm should be kept still, and no movement should be performed, especially during data acquisition.
The Newtom 5G XL CBCT machine (Verona, Italy) (Figure 2B) with native FOV 21x19 cm (extra FOV 21 cm diameter and 22 cm height) has already been applied for highly detailed investigations in orthopedics, otorhinolaryngology, maxillofacial surgery and dentistry (16). Recently, the Newtom 7G 3D CBCT is now being used in veterinary for assessment of animals’ extremities and lung. Although additional COVID-19 positive patients have not been identified through this method so far, the large field of view and supine position may enable the physician to evaluate the thoracic area. The major limitation of CBCT compared to MDCT is: longer scanning times which may result in significant lower image quality if there is movement (susceptibility to motion artifact) during 3D acquisition. Novel methods, providing faster scanning time or larger FOV, will efficiently reduce this artifact. In addition, if applicable, the patient is put into apnea or asked to hold the breath for less than a minute. Lewis et al provided a method to reduce motion artifacts from CBCT scanning. Another limitation is that CBCT is inefficient in accurate soft tissue evaluation, therefore CBCT with the injection of IV contrast medium is also not practical in assessments of soft tissue pathologies. Although CBCT has lower contrast resolution than MDCT and therefore lacks the ability to accurately present a Hounsfield Unit, it is still suitable in evaluating the opacifications and consolidations within lung lobes. Not all modern CBCT scan provide a supine position of a field of view large enough to depict lungs. RT is an effort to detect pulmonary changes suggestive of COVID-19 pneumonitis. Given that imaging characteristics have been shown to correlate with clinical severity and progression of disease, the combination of clinical and laboratory findings and acquaintance with typical radiographic COVID-19-related changes.
As many patients with cancer undergo routine CBCT during RT, familiarity of radiation oncologist to stay alert on thoracic imaging to check for typical CT changes of COVID-19 pneumonitis is advisable (20).
Conclusion
Regarding the everyday increase in the number of patients confirmed with COVID-19, augments the need for a safe and efficient imaging modality. The technology of CBCT is useful in imaging high subject contrast anatomies such as lung and provides a three-dimensional scan with significant lower patient radiation dose. Therefore, when used with a large FOV in supine position, may in part be a sufficient screening method.
Ethics approval
Ethics approval was not required as the patients were assessed during their routine radiotherapy treatments. However, informed consent from cases were obtained.
Consent for publication
All authors have provided consent for publication.
Availability of supporting data
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Conflict of Interest
None declared.
Funding
This research received no specific grant from any funding agencies.